Code green: Shrinking healthcare’s carbon footprint
By MaRS Staff | April 7, 2026

Decarbonization in Action is working to make healthcare kinder to the planet without compromising the quality of care for patients.
It’s a familiar sight in a doctor’s office. A strip of paper laid over the examination table. A thin but reassuring barrier between your body and those which came before.
There’s just one wrinkle: it’s mostly pointless.
“There’s limited evidence that it serves any purpose, really, except for making you feel like you’re at the doctor’s office,” says William Gagnon, director of implementation at the Canadian Coalition for Green Health Care (CCGHC), a non-profit that brings together more than 400 healthcare workers and organizations and has been supporting sustainability initiatives for 25 years.
The persistent paper is both a symptom of the slow progress in shrinking healthcare’s substantial environmental footprint and a sign of the enormous opportunity for change.
Healthcare accounts for around 5 percent of Canadian carbon emissions. That’s partly because of the system’s scale. Canada has more than 700 hospitals, which must be heated or cooled around the clock, often using natural gas. More than 2 million surgeries are performed every year, generating vast quantities of surgical waste, such as single-use gloves and masks. And every day, thousands of patients must be fed and linens cleaned.
It’s also because progress to decarbonize healthcare has been slow. Protected by its status as an essential service, healthcare has faced less scrutiny over its sustainability practices than other large industries. That means climate action is rarely top of the agenda in a highly regulated system where patient care comes first, staff are stretched thin and budgets are always tight.
“Implementing sustainability in healthcare is difficult because there’s a lot of competing priorities,” says Gagnon, who is also executive director of the Northwest Territories Medical Association. “I hear from my members that they are burned out, they have too much work and they can’t leave work at 5 p.m. because they have so many emails to sift through and charts to finish.”
But as physicians see growing numbers of patients affected by climate disasters like wildfires, pressure to change is growing from within.
There is plenty of low-hanging fruit still on the decarbonization tree according to Vivian Shi, a project manager at CCGHC: “There are a lot of impactful solutions that can be readily taken up and don’t affect patient outcomes.”
For instance, asthma pumps that use propellant gases can be switched for dry-powder inhalers. Acetaminophen given by intravenous drip can be replaced with pills, which use less single-use plastic and create only one-twelfth of the carbon emissions in their manufacturing. And during surgeries, anesthesiologists can choose alternative analgesics to desflurane, which is such a potent greenhouse gas that one bottle is equivalent to burning 440 kilograms of coal. As awareness of desflurane’s drawbacks has risen, hospitals have started phasing it out. CCGHC estimates that eliminating its use across Canada would save the equivalent of 153,000 tonnes of carbon emissions annually.
To encourage the adoption of solutions, CCGHC launched Decarbonization in Action in April last year. Funded by the Peter Gilgan Foundation and supported by MaRS, it aims to help the healthcare sector in the GTHA avoid 500 tonnes of emissions over the course of the project. It has identified 25 decarbonization initiatives where it can provide technical support, including performing the complex calculations required to determine emissions reductions.
Victoria Brzozowski, a sustainability manager and former environmental lead at Hamilton Health Sciences (HHS), says that collaborating with CCGHC not only enabled the hospital system to move more quickly than it could have alone, it also helped to measure the impact of those changes. “Working by yourself is incredibly limiting, but the Coalition brings additional resources, qualifications and creative thinking.”
Here are some initiatives Decarbonization in Action has supported to make healthcare kinder to the planet without compromising the quality of care for patients.
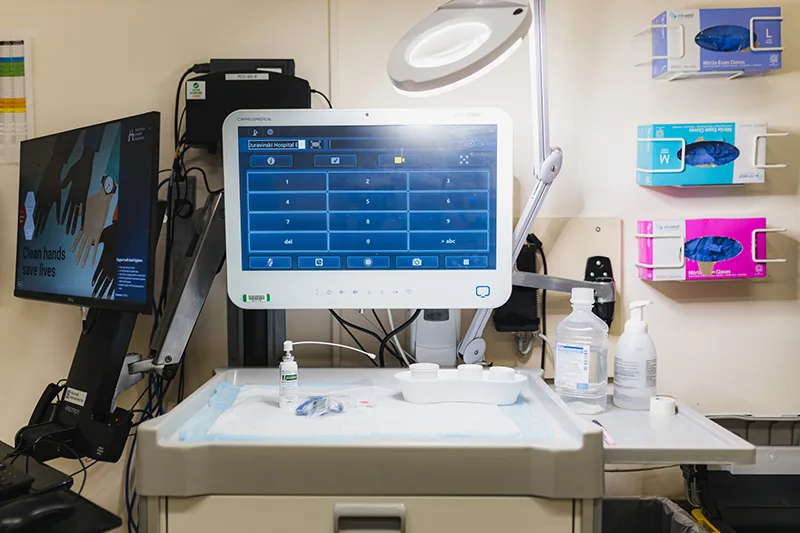
By switching to tap water for regular endoscopies, Hamilton Health Sciences avoids more than 25 kilograms of plastic waste each month.
Switching to a greener alternative
Endoscopies are common procedures for checking a patient’s digestive system for signs of disease. HHS, one of the country’s largest academic health sciences centres, performs 18,000 of them annually. Doctors insert a camera on a flexible tube down the patient’s throat to navigate through the stomach and gut. To give a clear view of the tissues, the endoscope shoots a jet of water ahead of it. “It’s like a power wash for the inside of the colon, so you can see polyps and lumps and bumps,” says Dr. David Armstrong, a gastroenterologist at McMaster University and HHS.
Until recently, HHS used bottled sterile water during the procedure. Most other hospitals have done the same since an influential paper advised it in the 1980s. But over the past decade research has shown that sterile water is not needed after all, not least because the patient drinks regular tap water before and after their endoscopy, so why not use it during the procedure too? “There was never any proof that sterile water was necessary, but once somebody decided it was, it’s very difficult to prove you don’t need it,” says Armstrong.
With the plastic sterile water bottles contributing to the 2 kilograms of waste produced by the average endoscopy procedure, some physicians have been calling for change. One of those is Dr. Meghan Bourque, a surgical resident at McMaster and HHS who pushed for a switch to tap water and reusable bottles as part of a course she was taking on championing sustainability in healthcare. Dr. Bourque, together with Sandra Alexander and Tipu Islam, launched a pilot project as part of the Circular Clinical Care project at CCGHC, which was made possible with an investment from Environment and Climate Change Canada.
“In many areas of healthcare where changes make sense, people ask why don’t we just do it? It needs all the appropriate people on board so they either endorse it or they’re not blindsided by it,” says Dr. Armstrong, who also serves on the Canadian Association of Gastroenterologist’s Climate Change Committee. “It’s a question of defining what you want and then giving people time to work it out.”
In this case, that involved seeking approval from a long list of groups including gastroenterology physicians, HHS’s risk management team and the endoscope manufacturers. Nobody objected. Brzozowski attributes that to the growing awareness among healthcare professionals of environmental issues. “In a survey, 80 percent of our staff said they think of the environmental impact they’re having while providing care,” says Brzozowski.
Physically making the switch to tap water for regular endoscopies was straightforward, although HHS continues to use sterile water for complex cases and children. CCGHC and HHS calculate the move avoids nearly 25 kilograms of plastic waste and 34 kilograms of carbon emissions monthly.
Cutting down waste
Dialysis is a life-saving treatment for patients with kidney disease. But it is also one of the more resource-intensive healthcare procedures. Removing toxins from a patient’s blood requires a complex mixture of acid concentrate (electrolytes), bicarbonate and purified water. At some hospitals, the acids are delivered in single-use containers, creating a mountain of plastic waste. In addition, not all the acid is used during a standard four-hour dialysis treatment. Because hygiene rules prohibit remaining acid being given to the next patient, up to 1.5 litres are poured down the drain after every treatment.
St. Michael’s Hospital in downtown Toronto took a different approach. The hospital’s clinical engineering technologists, Hassan Pooya and Simranjet Singh recently redeveloped a centralized acid delivery system, which distributes acid to its 35 dialysis stations. Originally constructed in 1993 when it could supply only a single type of acid, the system has been expanded with additional lines. Today, it can pipe four different acids to each dialysis station from 800-litre tanks that stand in a small room near the nephrology department. Because unused acid recirculates back to the tanks, waste is dramatically reduced.
“We are not even wasting one litre of acid a month,” says Hassan Pooya, a clinical engineering technologist who has worked on the delivery system since its inception.
A similar system operates at St. Michael’s satellite dialysis unit in East York Town Centre. CCGHC has calculated that between the two sites, the system saves nearly 95,000 litres of acid and 2,100 kilograms of plastic, while avoiding 28 tonnes of carbon emissions a year.
Clinical engineer technologists at St. Michael’s designed and built components for both systems themselves because they struggled to find cost-effective commercially available options. Though undoubtedly an act of brilliance, it underscores how frequently sustainability initiatives in healthcare rely on a handful of committed individuals to innovate and push through change.
Scaling decarbonization
CCGHC is hoping to make it easier for healthcare workers to adopt sustainability measures by sharing knowledge more broadly.
“I speak to physicians every week who want to do something. But every practice is different, the sources of greenhouse gas emissions under every specialty are different. They don’t teach climate change or decarbonization in med school, and physicians often feel like they don’t know where to start; because there is so much to do,” says Gagnon.
CCGHC’s answer is to create a database of climate solutions that are proven and ready to deploy. Called the Solutions Atlas, it collates evidence-based sustainability initiatives that have been implemented in healthcare settings in Canada and around the world.
So far, more than 40 solutions have been entered in the database. These encompass a broad range of initiatives, such as LED lighting retrofits, introducing reusable gowns, minimizing unnecessary tests and adding sustainability requirements into procurement contracts.
The Solutions Atlas provides tools for users to zero in on solutions applicable to their specialty area and to assess the ease of implementation and their likely impact. It also lists names of practitioners who have already adopted these measures and can act as expert guides.
“Healthcare is highly risk averse,” says Shi. “A lot of people need to see that other hospitals have done something in a Canadian context to be convinced that it’s feasible.”
The database will launch publicly by the summer if funding can be secured.
Gagnon sees its likely audience as mid-career doctors who are looking for a new challenge and have enough clout in their organization to drive change. He wants the Atlas to be more than a centralized place where physicians can learn about potential solutions. He hopes it will convince doctors and hospital administrators that they don’t need to perform their own pilot projects but can begin making change at scale — or as he puts it, shifting doctors’ mindsets from performing peer review on these ideas to exerting peer pressure for change.
“People have spent a lot of time researching and developing and testing these solutions,” he says. “Now we just have to share them and show others that they work.”
This article was created in partnership with the Canadian Coalition for Green Health Care. Find out more about its initiatives here.
Images courtesy of Hamilton Health Sciences
 MaRS Staff
MaRS Staff